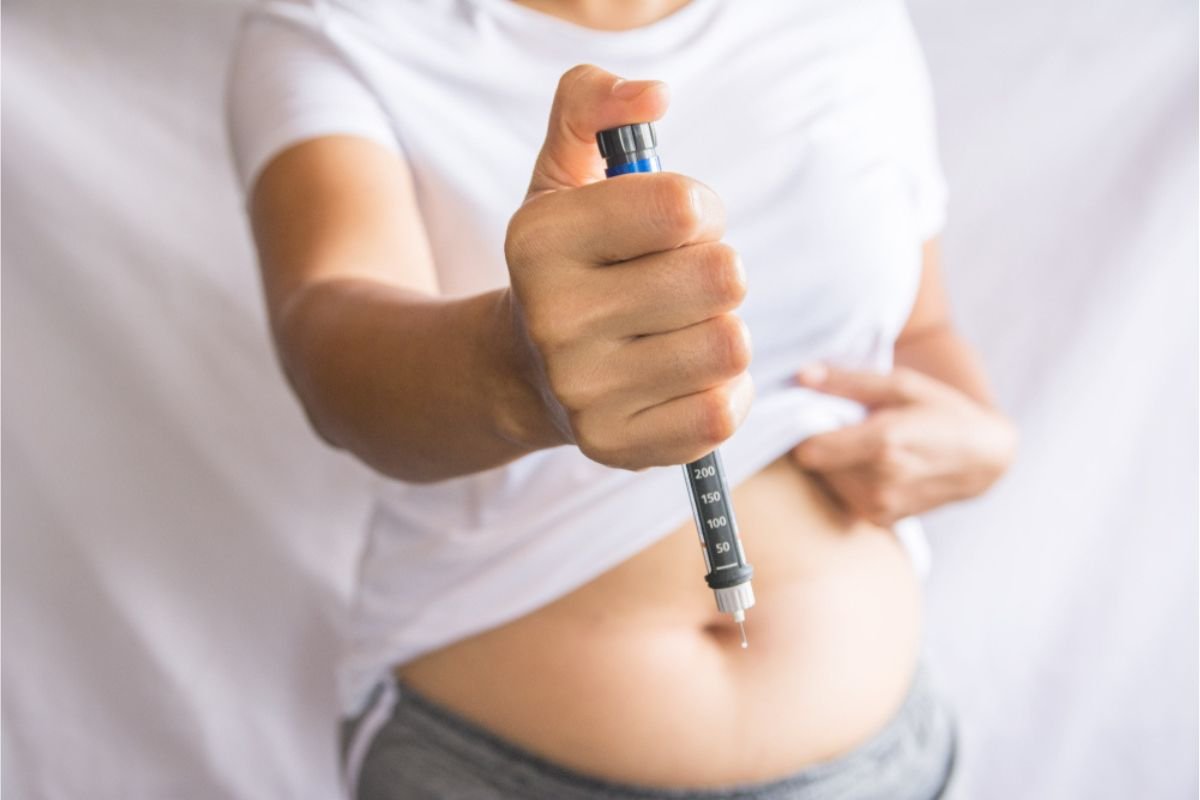
Are you struggling to shed those extra pounds and looking for an effective weight-loss solution? Well, you’re not alone! Losing weight can be difficult, but having the right tools and support makes this journey easy.
One such tool that has gained attention in recent times is Wegovy. But what exactly is Wegovy, and Does United Healthcare cover Wegovy for Weight loss?
In this article, we’ll explore all the details about Wegovy and how insurance coverage may affect your weight loss journey.
What is Wegovy?
Wegovy is a prescription medication making waves in the weight loss community. It is an injectable drug that contains semaglutide, which works by simulating a hormone in the body called GLP-1. This hormone helps regulate appetite and food intake.
It is still not known that Wegovy® is safe and effective when taken with other medicines, over-the-counter, or weight loss products. One of the key benefits of Wegovy is its ability to help people lose weight and keep it off.
Clinical trials have shown that individuals who took Wegovy experienced significant weight loss as compared to those who took a placebo. In fact, many members lost an average of 15% of their body weight over the course of one year.
Read on if you want to learn more about whether United Healthcare covers Wegovy for weight loss or how to get insurance coverage for this medication.
Related: Does wegovy affect menstrual cycle? Uncover the Truth
Does United healthcare cover wegovy for weight loss?
The good news is that United Healthcare does cover Wegovy for weight loss, but the coverage can vary depending on the specific plan that you choose.
Check your insurance policy or contact United Healthcare for coverage for prescription weight loss medications like Wegovy. Mostly, people do not read the instructions carefully and just submit them. They can provide you with information about any requirements or restrictions that may apply.
Keep in mind that even if your plan covers Wegovy, there may still be some out-of-pocket costs, such as deductibles or co-pays. It’s important to review your plan details carefully and consider contacting the Wegovy manufacturer for assistance programs or discounts.
Also Read:
- Does Blue Cross Blue Shield Cover Mounjaro for Weight Loss?
- Does Blue Cross Blue Shield Cover Wegovy for Weight Loss?
How much does Wegovy cost with or without insurance?
The cost of Wegovy with insurance depends greatly on the specifics of your plan. However, according to the drug’s manufacturer, Novo Nordisk, without insurance, the cost for Wegovy is around $1,300 per month. That’s why it’s important to have insurance to help cover these costs.
If you have United Healthcare insurance, make sure to reach out to them directly to get the most accurate information about what your plan covers and any costs you might have to pay. They can provide you with the specifics regarding co-pays, deductibles, and any pre-authorization requirements for Wegovy.
In the event that your insurance does not cover the entire cost of the medication, Novo Nordisk offers a savings card that can help eligible patients save on their Wegovy prescription. Please visit NovoCare® for more information about this program.
It’s also worth noting that the price of prescription medications can vary by pharmacy, so it may be beneficial to compare prices at different pharmacies in your area.
What is the cost of Wegovy on United Healthcare Plans?
As per the United Healthcare’s Prescription Drug List (PDL), the cost of Wegovy varies depending on the specific plan you have opted for.
Usually, Wegovy falls under Tier 3 (Non-preferred brand name) or Tier 4 (Specialty medication), which means you’ll likely have a co-pay or co-insurance amount to pay. It’s pertinent to keep in mind that prior authorization may be required for this medication. You can refer to the United Healthcare’s PDL document for more detailed information.
Another reliable source to check out is the NovoCare® Savings Card website. Depending on eligibility, it allows you to pay as little as $25 for a 28-day supply of Wegovy for up to 24 months. This can be a substantial savings for many individuals.
Lastly, you can use the GoodRx website to compare prices at various pharmacies in your area. They provide updated price estimates for Wegovy with and without insurance, helping you make an informed decision on where to fill your prescription.
Explore diverse weight loss solutions that go beyond Wegovy
If you’re looking for other options instead of Wegovy, there are different services and treatments available for weight loss. Here are some of them:
- Exercise and a healthy diet are key for weight loss. Being active burns calories, boosts metabolism, and improves health. Eat fruits, veggies, lean proteins, and whole grains to sustain weight loss.
- Cognitive-behavioral therapy (CBT) can often play a vital role in weight loss. It helps people to identify and change negative thought patterns that lead to unhealthy eating habits, thereby fostering a healthier relationship with food.
- Prescription weight loss medications should be considered as part of an overall weight loss strategy and not a standalone solution. They are usually recommended for those with a BMI of 30 or higher, or 27 or higher with a weight-related health issue.
- Bariatric surgery may be an option for severe obesity (BMI 40+), or BMI 35+ with weight-related health issues. Keep in mind, these surgeries require lifelong commitment to lifestyle changes and regular medical check-ups.
- Stay updated on weight loss research through organizations like NIDDK and ASMBS. They offer valuable resources on this topic.
- Weight loss apps and digital platforms can provide useful tools to track your progress, get nutrition advice, and stay motivated. Some popular platforms include MyFitnessPal, WW (formerly Weight Watchers), and Noom.
Related: Does Cigna Cover Bariatric Surgery? Complete Guide
Addressing Common Concerns about Wegovy
Wegovy, like any medication, can have side effects. The most common ones include nausea, diarrhea, constipation, and abdominal discomfort. However, these side effects usually decrease over time as your body adjusts.
According to the FDA, Wegovy has a “black box warning,” the most serious type of warning for prescription drugs, because of the potential risk of thyroid C-cell tumors.
Studies in rodents showed an increased risk of tumors especially thyroid C-cell tumors with the use of semaglutide, the active ingredient in Wegovy, although it is not known whether Wegovy would cause these tumors in humans.
Before you start taking Wegovy, make sure you discuss with your healthcare provider about any pre-existing medical conditions like pancreatitis, gallbladder disease, or kidney disease, as Wegovy may worsen these conditions.
Keep in mind that Wegovy should not be used in combination with other semaglutide-containing products or with other GLP-1 receptor agonists.
Remember to always consult your healthcare provider or a pharmacist for accurate information about Wegovy. For more details, you can refer to the FDA’s prescribing information guidelines for Wegovy.
How to check your wegovy coverage?
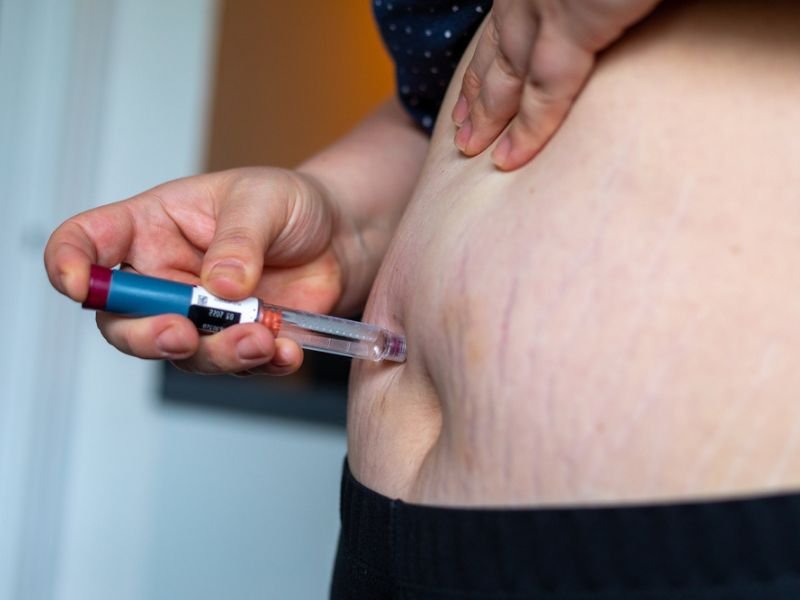
Follow these steps to determine that if your Wegovy is covered by United Healthcare insurance.
- Review your Insurance Documents: Check your United Healthcare insurance policy or contact your insurance provider to see if Wegovy is covered. Look for details about coverage for weight loss prescription medications.
- Meet Specific Criteria: Sometimes, coverage requires certain criteria like a specific body mass index (BMI) or your doctor’s recommendation for Wegovy as part of a weight loss plan.
- Meet Healthcare Provider: Talk to your doctor. They can guide you through the coverage process, help with paperwork, and provide necessary documents.
- Alternatives: Even if Wegovy isn’t covered, your insurance might offer other options to support your weight loss goals.
- Insurance Differences: Keep in mind coverage can vary based on location, plan type, and individual policy terms.
How to get insurance coverage for wegovy?
If you see that your United Healthcare insurance doesn’t cover Wegovy for your weight loss or if you face any coverage restrictions, you can try these steps to possibly get the medication covered:
- Know Your Policy: Stay informed about your insurance and plan details. Some insurance companies have different coverage rules, so take time to read and understand your policy.
- Talk Your Doctor: Discuss with your healthcare provider about getting “prior authorization” for Wegovy. This means your doctor explains why you need this medication and asks your insurance for approval.
- Get Professional Support: Sometimes, you might need papers from a registered dietitian or other medical experts to show them that Wegovy is important for your weight loss plan.
- Prepare for Costs: Even if your insurance agrees, there could still be expenses for you. This depends on things like deductibles, co-pays, and some limits set by your insurance.
- It Can Take Time: Getting insurance coverage for Wegovy might not be easy, and sometimes it requires more time for approval. But with knowledge about your policy and help from healthcare pros, you can improve your chances of getting coverage for this weight loss medicine.
Eligibility criteria for Wegovy
To qualify for Wegovy coverage under United Healthcare, you generally need to meet certain eligibility criteria.
These may include a diagnosis of obesity (a body mass index, or BMI, of 30 or more) or overweight (BMI of 27 or more) in combination with a weight-related health issue like high blood pressure or diabetes.
A prescription from your provider is also required. Keep in mind that these are general guidelines, and specific criteria may vary by plan. It’s critical to consult with your doctor and insurance company to understand your eligibility for Wegovy coverage.
Whether or not your health insurance covers Wegovy will determine its availability. If you don’t have insurance, Wegovy can be expensive, but the manufacturer provides a savings program to assist eligible patients in saving money.
Plus, Wegovy is intended to be a part of a long-term weight management plan that includes a reduced-calorie diet and regular physical activity. It is not a quick fix but rather a tool to help facilitate sustainable lifestyle changes.
Factors About To Determine The Coverage
There are some main factors on which your coverage for weight loss may depend:
- Policy Details: Your specific insurance policy plan plays a big role in deciding what is covered.
- Medical Need: Insurance often covers medically necessary things, so the need for Wegovy in your case is important.
- Doctor’s Recommendation: If your doctor recommends Wegovy as part of your treatment, it could impact coverage.
- Treatment Guidelines: Sometimes, insurance follows specific guidelines for what they cover, which can affect Wegovy’s coverage.
- Policy Changes: Changes in your insurance policy can also change what is covered over time.
Also Read: How To Reconstitute Semaglutide: A Complete Guide
Conclusion
In conclusion, Does United Healthcare cover Wegovy for Weight loss? Yes, United Healthcare covers Wegovy in most cases, but it’s also essential to verify the specifics with your insurance provider and understand any potential costs involved. Consulting with your healthcare provider will also help you determine whether this medication suits you based on your circumstances and goals.
FAQ
Does United Healthcare cover weight loss medication?
Yes, United Healthcare covers a variety of weight loss medications. The type and amount of coverage depend on your plan. In general, most of the plans will cover drugs that are approved by the FDA for long-term use and other medically required medications under certain conditions.
Is semaglutide covered by United Healthcare?
Yes, semaglutide is usually covered by United Healthcare. However, coverage can depend on specifics like the patient’s medical necessity, recommendations from healthcare providers, and individual plan details. Some plans might require prior authorization, meaning your doctor will need to confirm why the medication is essential for your treatment.
Will my doctor prescribe Wegovy for weight loss?
Yes, it’s possible that your doctor will prescribe Wegovy for weight loss if they determine that it’s the best course of treatment for your specific situation. Doctors generally see some factors like your overall health, any underlying medical conditions, BMI, and your previous attempts at weight loss.
How much weight can you lose in two months with Wegovy?
The weight you can lose with Wegovy varies based on factors like starting weight, diet, exercise, and medication adherence. Clinical studies have shown that on average, people who took Wegovy for 68 weeks lost 17% of their initial body weight. In a shorter duration of two months, some patients have reported losing approximately 5-10% of their starting weight. The actual numbers may vary.
What is the success rate of Wegovy?
The success rate of Wegovy is generally high, but it can vary for every person due some factors. In clinical studies, nearly 75% of people who took Wegovy lost at least 5% of their initial body weight after 68 weeks. More impressively, about one-third lost 20% or more.
Does United Healthcare cover weight loss injections?
United Healthcare’s coverage for weight loss injections can vary depending on your specific insurance plan and the type of injection. However, checking with your insurance provider for accurate and up-to-date coverage information is recommended.
According to the United Healthcare “Medications for treating obesity are covered only if they fall under the supplemental pharmacy benefit and are approved as medically necessary for extreme obesity.”
Does United healthcare cover mounjaro for weight loss?
Yes, it may cover medications like Mounjaro for weight loss or diabetes. Remember, the coverage and expenses can differ based on the specific plan you have with United Healthcare Medicare Advantage. It’s best to review your plan’s details for accurate information.
Does United Healthcare cover ozempic for weight loss?
Ozempic is an injection that is taken weekly to help the pancreas produce more insulin, which lowers blood sugar levels. Some doctors may prescribe it but still, it’s not officially approved for weight loss.
If we talk about coverage by United Healthcare it’s recommended to check with United Healthcare directly or review your insurance policy documents. Because it can vary based on your specific insurance plan.
Does uhc cover wegovy?
Yes, UHC covers Wegovy but the coverage can vary depending on the specific plan that you choose.
Check your insurance policy or contact UHC to clarify the coverage related to prescription weight loss medications. Mostly, people submit instructions without careful reading and missing the important requirements or restrictions.

Dr. Usman is a medical content reviewer with 12+ years of experience in healthcare research and patient education. He specializes in evidence-based health information, medications, and chronic health topics. His work is based on trusted medical sources and current clinical guidelines to ensure accuracy, transparency, and reliability. Content reviewed by Dr. Usman is for educational purposes and does not replace professional medical advice.